Gram Stain –Pus:
Why Gram Stain (Pus) Test?
CLINICAL INFORMATION
Skin is the largest organ present in the human body. It serves as an anatomical barrier between sterile internal organs and the external environment (pathogenic microbes). A breach in the skin or mucosal surface (eg. bites, trauma, surgery or diseases) may result in skin or soft tissue infections that may spread around or eventually to other parts of the body if untreated. Pus is a natural part of the healing process of suppurating wounds. Pus is a sign of an infected wound and the body’s defence mechanism (immune system) fights against the invading infection and heals the injury (wound healing). Pus is a thick, foul odour and usually yellowish or greenish (colour depends on the location and type of infection) opaque fluid (protein-rich fluid: Puris) produced in the infected site of the tissue which contains a collection of infectious dead microbes, dead WBCs, tissue debris like remains of dead cells – infected host cells and serum etc. Complications of un-drained pus include skin abscess, fistula (abnormal communication between two parts such as organs, blood vessels and another structure eg. blind type and/or complete type of fistula), the spread of infection to the surrounding areas (invasive spread), recurrence of infection, systemic infection, sepsis etc. Examples of pyogenic bacteria include Staphylococcus species, E Coli, Klebsiella pneumonia, Salmonella typhi, Pseudomonas aeruginosa, Neisseria gonorrhea, Actinomyces, Burkholderia mallei, Mycobacterium tuberculosis etc. Fungal infections include tinea pedis (athlete’s foot), Histoplasma, candida, actinomycetes etc that can cause from site of wound infection to dispersive type known as mycotic mycetoma. Complications due to prolonged pyogenic infections can lead to impetigo (usually in children), osteomyelitis, septic arthritis, necrotizing fasciitis etc. Clinical manifestations of an infected wound include signs of inflammation (rubor – redness, tumour – swelling, calor – heat, dolor – pain and loss of function), pus or bad-smelling /odourless fluid drain from the wound, boils, rashes, pustules etc and in case of systemic manifestation it shows the signs and symptoms of fever, fatigue, chills, confusion etc. Culture and Sensitivity test in Pus Specimen facilitates to the treatment of wound infection. This test helps to determine if a wound is infected (presence of the pathogenic organism in positive culture results shows an infected wound), to reveal the type of infection (eg. bacterial – aerobic in case of open wound or anaerobic bacteria in case of punctured closed wound, gram-positive or gram-negative strains – based on the presence of cell wall, fungal infection etc) and to establish best possible medication to treat the infection – susceptibility testing (A clear circular halo known as plaque or zone of inhibition (antibiotic has inhibited the growth or killed the colonies of harmful pathogens) appears around the antibiotic disc indicates the absence of bacteria). This helps in the discrimination of type of antibiotic treatment such as broad-spectrum / narrow-spectrum antibiotics to heal the wound (in case of bacterial resistance to antibiotics, if no discernable plaque/zone of inhibition is found around filter paper with antibiotic hence effective medication is prescribed). If the culture result is negative it shows a sterile wound (free from pathogenic microbes). This pus swab culture and sensitivity test are ordered in cases of conditions such as patients with delayed wound healing, risk of spread of infection to the surrounding areas causing secondary complications affecting another organ (s) or organ systems, allergies, causing systemic manifestations, co-morbid and/or underlying medical conditions like diabetes, hypertension, vascular diseases like DVT, sepsis etc and to avoid further complications. Other tests include blood tests to check CBC, use of Mass Spectrometry using Matrix-Assisted Laser Desorption Ionization Time Of Flight – MALDI-TOF to identify and confirm the genus and species of a bacterial colony grown on culture medium within half an hour, tests for fungal infection, liver function, blood sugar and proteins (antibodies using ELISA), urine tests, aspiration fluid (ascites) or tissue biopsy in deeper wounds (fungal spores etc) or sample specimen (sputum, blood, urine etc) collected from other suspected sites (bone marrow specimen in osteomyelits etc) for histopathological studies, PCR etc. Gram stain also called as Gram stain method used for staining to classify two groups of bacterial species such as gram-positive and gram-negative bacteria. This term Gram stain is derived from the Danish bacteriologist Hans Christian Gram who developed this technique. Gram staining differentiates bacteria by the physical and chemical properties of the bacterial cell wall. Bacteria with gram-positive cell walls have thick peptidoglycan which retains the primary stain crystal violet and Lugol’s iodine solution is added to strengthen the bonds of the stain. While the gram-negative bacteria since they have a thinner bacterial cell wall allow the crystal violet to wash out on the addition of ethanol, hence their cell membrane is stained pink or red by the counterstain (safranin or fuchsine).
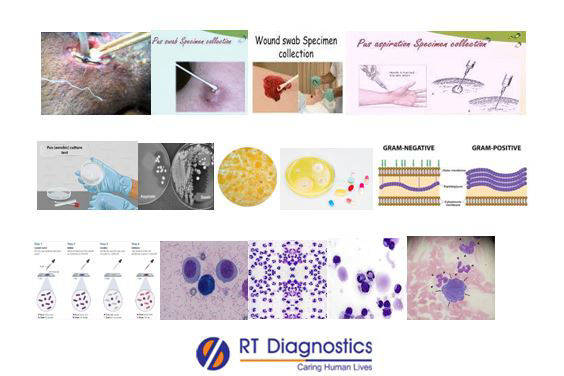
General Instructions:
Sample Requirement: Specimen –pus (As guided by the physician). Test Preparation: None.
NOTE - Sample for specimen collections may vary based on the patient’s condition/cases according to the patient’s presenting complaints/signs or symptoms:
SPECIMEN REQUIREMENT (Special or Rare Cases) - As instructed and guided by Physician / Clinician / Pathologist / as per Laboratory’s requirements, according to procedures and protocols.
This Multi-Specialty Clinical Referral Laboratory RT DIAGNOSTICS provides precise and accurate tests with an extensive range of testing services to the medical centres to help in the diagnosis and identification of pathology in the test specimens for infectious diseases and also to evaluate the function of organ systems of the patient. It prevents further complications and helps to stabilize and restore health to near normalcy at the earliest without delay.



