Gram Stain – Pleural Fluid:
Why Gram Stain (Pleural Fluid) Test?
CLINICAL INFORMATION
Pleura are a membrane lining the thoracic cavity (parietal pleura) and covering the lungs (visceral pleura). The parietal pleura folds back on itself at the root of the lung to become the visceral pleura. A small amount of space between the two pleurae and lubricating fluid at their contact points allow the lungs to expand. The pleura exude a thin fluid that keeps it moist and lubricated. Thus the pleura with two thin layers of tissues protect and cushion the lungs. The pleural fluid lubricates the pleural cavity so that the pleural tissue can slide against each other. Most common causes of lung and pleural injuries include injuries of the chest (physical trauma), viral, fungal, bacterial causes of pleural effusion are due to Streptococcus milleri group, Streptococcus pneumonia, Streptococcal aureus etc and also by autoimmune diseases, rheumatoid arthritis, tuberculosis etc. Symptoms for pleural effusion include chest pain, dry and non-productive cough, dyspnea, orthopnea etc. Thoracentesis is a procedure where the needle is inserted through the chest wall into the pleural space to remove fluid or air from around the lungs. Pleural fluid testing is used to help diagnose the cause of fluid build-up in the chest (pleural cavity) which includes fluid appearance, cell count and fluid protein, albumin or LD level. The common complication of thoracentesis is pneumothorax, excessive bleeding while specimen collection, re-accumulation of fluid in the lung, infection at the site of thoracentesis, respiratory distress or breathing difficulties etc.
Culture and Sensitivity – Pleural Fluid Specimen test: This test specimen of Pleural fluid examines the aspirated fluid sample specimen from the pleural space in case of suspected infection and/or to diagnose the cause of fluid build-up in the space of the chest wall (for differential diagnosis to differentiate between exudates and/or transudate). Inflammation of the pleura causing exudates include infections, bleeding (bleeding disorders, trauma, pulmonary embolism, lung diseases eg. Sarcoidosis) and other causes like heart surgery, heart or lung transplant, pancreatitis and/or abscess in the abdomen etc. The non-infectious causes behind pleural effusion also include transudate (due to altered levels in the protein i.e low protein levels in the blood and/or due to injury or inflammation to the pleura - an imbalance between the pressure of the liquid within the blood vessels, drives fluid out of blood vessel), due to congestive heart failure or cirrhosis, tuberculosis, sarcoidosis, lung cancer, metastatic cancer, lymphoma, mesothelioma, RA, SLE etc. Other tests on pleural fluid other than culture and sensitivity include measurement of pleural fluid, estimation of biochemical parameters such as glucose, lactate, amylase, triglyceride, tumor markers such as CEA etc. Additional supporting tests include CBC, Chest X-Rays, CT Scan, Gram stain, fungal test, stool test for cysts in parasitic infestation, AFB test and adenosine deaminase to detect tuberculosis etc. Gram stain also called as Gram stain method used for staining to classify two groups of bacterial species such as gram-positive and gram-negative bacteria. This term Gram stain is derived from the Danish bacteriologist Hans Christian Gram who developed this technique. Gram staining differentiates bacteria by the physical and chemical properties of the bacterial cell wall. Bacteria with gram-positive cell walls have thick peptidoglycan which retains the primary stain crystal violet and Lugol’s iodine solution is added to strengthen the bonds of the stain. While the gram-negative bacteria since they have a thinner bacterial cell wall allow the crystal violet to wash out on the addition of ethanol, hence their cell membrane is stained pink or red by the counterstain (safranin or fuchsine).
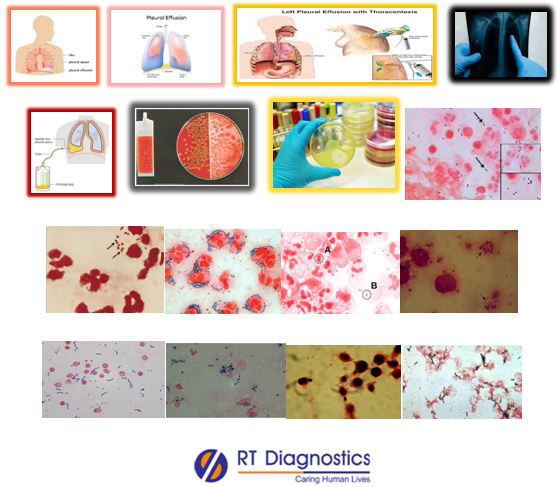
General Instructions:
Sample Requirement: Specimen – Pleural Fluid.Test Preparation: None.
NOTE - Sample for specimen collections may vary based on the patient’s condition/cases according to the patient’s presenting complaints/signs or symptoms:
SPECIMEN REQUIREMENT (Special or Rare Cases) - As instructed and guided by Physician / Clinician / Pathologist / as per Laboratory’s requirements, according to procedures and protocols.
This Multi-Specialty Clinical Referral Laboratory RT DIAGNOSTICS provides precise and accurate tests with an extensive range of testing services to the medical centres to help in the diagnosis and identification of pathology in the test specimens for infectious diseases and also to evaluate the function of organ systems of the patient. It prevents further complications and helps to stabilize and restore health to near normalcy at the earliest without delay.



